Overview
The term “mastectomy” refers to the surgical procedure performed to remove one or both breasts, either partially or completely. It is typically used to treat breast cancer, both in women and men, and there are several types of mastectomy that a surgeon can use:- Subcutaneous mastectomy - the surgeon removes the breast tissue, while preserving the nipple and areola
- Total or simple mastectomy - the entire breast tissue is removed, including the nipple and areola. If the cancerous cells have already spread to a nearby lymph node, that lymph node is also removed
- Modified radical mastectomy - not only the entire breast tissue is removed, but also the surrounding fatty tissue and lymph nodes.
- Radical mastectomy - it is similar to the modified radical mastectomy, but it is a more disfiguring procedure, since it involves the removal of the chest muscles associated with the affected breast. This surgery does not improve the survival rate in comparison with its modified version and it is rarely done nowadays.
- Skin-sparing mastectomy (lumpectomy) - breast tissue is removed through a small incision, which allows for the preservation of a higher amount of healthy tissue. This facilitates an eventual reconstructive surgery.
Advantages and disadvantages of mastectomy
Comparing conventional mastectomy with lumpectomy plus radiotherapy, the latter is preferable for those women who want to preserve as much breast tissue as possible. The mastectomy allows the patient to avoid the side effects of radiation and the chance of recurrence is very low.
Reasons for the procedure
The mastectomy can be applied to treat a number of breast cancers, including: noninvasive breast cancer, early stage breast cancer, locally advanced breast cancer (usually after chemotherapy to reduce the tumor’s size), inflammatory breast cancer, Paget’s disease of the breast and locally recurrent breast cancer.In spite of the growing number of conservative therapies for breast cancers, the mastectomy is still the best option for a certain group of patients:
- Women who have already undergone radiation therapy
- Women who have 2 or more cancerous growths in the same breast that are too far apart to be removed using only one surgical incision
- Pregnant women who need radiotherapy and cannot risk it because of the risks to the fetus
- Women who have certain connective tissue diseases and, as a consequence, cannot undergo radiotherapy
- Women with tumors that are more than 5 centimeters in size and that do not respond to chemotherapy
- Women who have undergone a lumpectomy with several other re-excisions and still have cancerous masses
- Women with cancerous growths too big in relation to their breast size
- Women with mutations in the BRAC1 and BRAC2 genes, as a prophylactic strategy, i.e., as a way to reduce the risk of developing breast cancer
- Male breast cancer patients
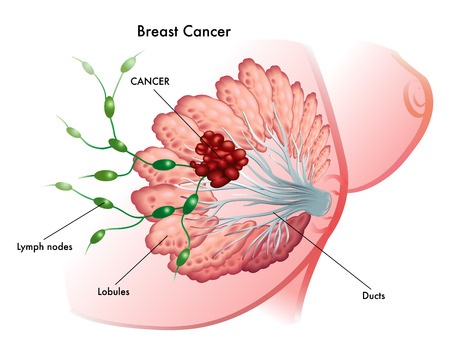
Risks of the procedure
The risks of a mastectomy are similar to the risks of any other surgical intervention and include the possibility of formation blood clots in the legs that may travel to the lungs, blood loss, breathing problems, infections (namely of the surgical wound), heart attack or stroke and adverse reactions to medications. There can also be scabbing, blistering or skin loss along the borders of the surgical cut.When the mastectomy performed is more aggressive (e.g. radical mastectomy), the risks include potential damage to the nerves that supply the arm, back and chest wall, swelling of the arm, shoulder pain and stiffness and a stinging sensation where the breast used to be.
When a lymph node is removed, there can be a feeling of numbness under the arm on the same side.
Contraindications for the procedure
A mastectomy is contraindicated in a number of cases and various factors come into play when a surgeon decides in favor or against this procedure. Among these, the stage and the type of cancer are very important variables. It is contraindicated, for example, in cases of locally advanced cancer that are inoperable, when the patient is old and fragile or the overall health state is too poor to sustain a surgical intervention.Consultation with a competent and experienced doctor will help to decide on the best individually suitable course of treatment.












