Overview
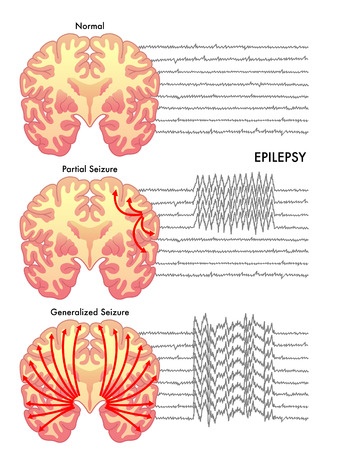
The term “Epilepsy” refers to a set of brain disorders characterized by the frequent occurrence of seizures. These seizures happen when a group of neurons (the cells that make up the brain) send out excessive and disorderly electrical signals.Seizures can be classified according to their cause and according to the part of the brain where they happen. They can be caused by many different factors which are not always known or identifiable. Depending on the part of the brain where the abnormal electrical activity took place, a seizure can be partial, generalized or secondary generalized (it started as a partial seizure, but it eventually progressed to both halves of the brain).
Genetic factors, head trauma, other brain conditions, infections, prenatal damages and developmental disorders are all possible causes of epilepsy.
Symptoms
The main characteristic of epilepsy is the long-term recurrence of seizures. Seizures do not look the same on all patients, so a number of symptoms can be identified in people with epilepsy, including:
- Uncontrollable jerking movements of the upper and lower limbs
- Loss of awareness for short periods of time during which the person is irresponsive
- Staring/blackout spells, after which the person has no memory of what happened
- Sudden loss of consciousness
- Stiffness of the body
- Sudden bouts of chewing or blinking
Risk factors
Some factors are known to increase the risk of epilepsy:- Age: epilepsy is more likely to begin in the childhood or after the age of 60
- Family history of epilepsy
- Trauma to the head (e.g. after a car accident or a sports injury)
- Stroke and other diseases affecting the blood vessels
- Dementia, especially in the older populations
- Infections located in the brain
- Long seizures caused by high fevers, especially in children (the risk is higher when this factor is coupled with other risk factors, such as family history of the condition)
Diagnosis
Getting an accurate family and medical history is one of the most important elements in diagnosing the epilepsy. If possible, the doctor should get input from people who have witnessed one of the patient’s seizures, so as to identify the type of seizures the patient is having.Tests that can be performed may include:
- A full physical and neurological exam that will allow for an evaluation of muscle strength, eyesight, hearing, reflexes, etc.
- Blood tests to evaluate the general biochemical parameters and organ functions. This will allow eliminating the possibility that the symptoms the patient presents are caused by other medical condition.
- Imaging studies of the brain, such as MRI scan.
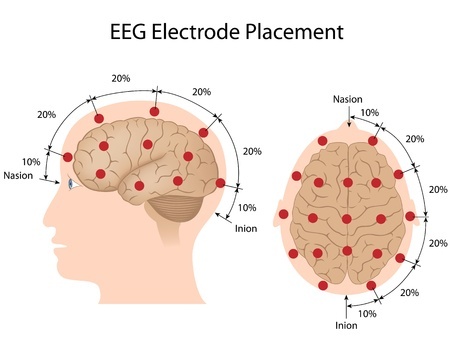
- An electroencephalogram (EEG), which analyzes the electrical activity of the patient’s brain. Since there is only a small chance that seizure would occur during the test, the results might turn out to be normal, even in people with epilepsy. Therefore, the prolonged EEG is generally used. This test is essential to confirm the diagnosis and identify the exact type of epilepsy that the patient is suffering from.
Treatment
Epilepsy is not a curable disease, but it can be managed. The main goal of treatment is to prevent the recurrence of seizures, thus allowing patients to lead an active and normal life.
- Medication - Anti-epileptic drugs are the most common treatment and the patient is normally required to take them for the rest of his or her life. Some patients do not respond immediately to therapy, and the trials of two or three different drugs might be necessary until the doctor identifies the most suitable treatment.
- Surgery - Brain surgery might be an option for patients for whom there doesn’t seem to be any effective drug. A very thorough evaluation is performed before a patient is considered suitable for a surgical approach, which happens to be more commonly used to treat the partial epilepsy.
- Diet - The adoption of a ketogenic diet (a high-fat, low-carb diet) has received much attention from the medical community in recent years, since it showed some potential to reduce the seizures. Since the compliance with this diet might be complicated, it is used mostly in young children who do not respond to medication.
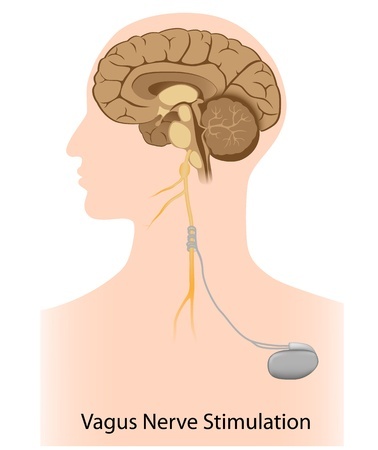
- Vagus nerve Stimulation - A more recent approach involves the insertion of a stimulator that will act on the vagus nerve. Although its implantation does not mean the person will not need any medication, it has been shown to reduce the seizure frequency by half in 40% to 50% of the patients.
The choice of the most individually suitable approach requires a careful examination of the patient’s condition and history. Experienced doctors are usually able to at least partially address the problem of seizures in most patients.










