Overview
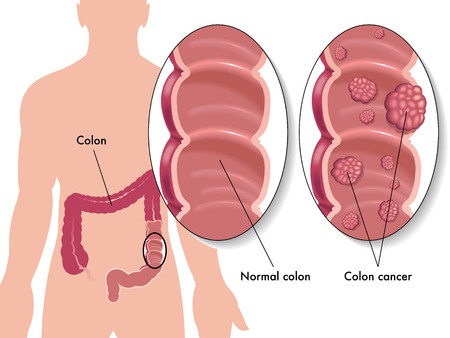
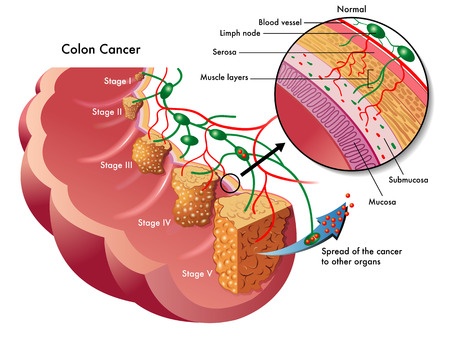
Colorectal cancer is a type of cancer that results from the uncontrollable growth and division of cells in the lower portion of the digestive system, namely in the colon and in the rectum. Frequently, colorectal cancer develops from benign clumps that grow in the intestine, named adenomatous polyps. For this reason, and to prevent colon cancer, screening for the identification and subsequent removal of polyps is recommended after the age of 50.Once it develops, colon cancer can spread to the adjacent lymph nodes and afterwards to more distant parts of the body, in the process known as metastasis.
Colorectal cancer is the third most commonly diagnosed cancer worldwide, being especially prevailing in the developed countries. It affects women and men alike.
Symptoms
In its initial stages, colorectal cancer may show little to no symptoms (this is one of the reasons why the screening tests are important). When they do appear, they are likely to be varied and depend on the cancer’s size and location. The most common manifestations include:
- Unexplained changes in bowel habits, including diarrhea and constipation
- The feeling that the bowels do not empty completely
- Blood or mucus in the stool
- Changes in the consistency of the stool
- Fatigue, weakness and weight loss
- Pain and discomfort in the lower abdomen, including gas and tenderness
Risk factors
There are various factors that increase the risk of cancer. These include:
- Age: colorectal cancer occurs much more frequently in people over the age of 50.
- A personal history of polyps
- A family history of colorectal cancer, namely if it has affected a direct family member (parent, sibling or child). If there are more than two members of the same family with colorectal cancer, the risk is even higher. However, this does not mean that the cause lays in a genetic abnormality – it can be due to a shared exposure to an environmental carcinogen
- Inflammatory intestinal diseases, such as ulcerative colitis and Crohn’s disease
- Inherited genetic syndromes, such as familial adenomatous polyposis
- A sedentary lifestyle and a diet low in fiber and high in fat and calories
- Diabetes
- Obesity
- Smoking and alcohol consumption
Diagnosis
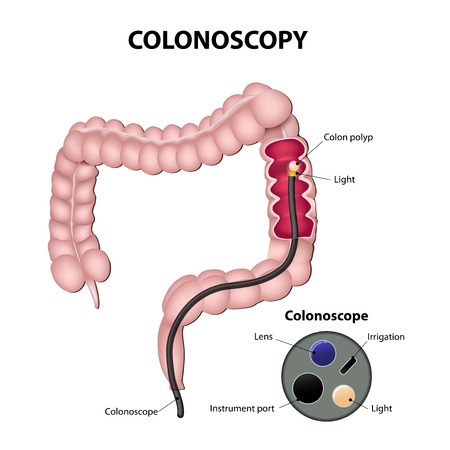
A doctor may suspect the presence of colon cancer after a routine digital rectal exam or on the basis of the patient’s complaints. A fecal occult blood test has the ability to detect very small, often not visible, amounts of blood in the stool. If this test comes back positive, a colonoscopy will be ordered. This procedure allows the doctor to observe the entire colon and rectum and, if any alarming masses are found, a small tissue sample will be collected. This sample will be analyzed under the microscope for the presence of cancerous cells.Once the diagnosis is confirmed, other tests will be done to assess if the cancer has spread. These include CT or MRI scans of the abdomen, pelvic area, chest or brain. Sometimes, PET scans are also used.
Treatment
Treatment depends on many variables, particularly the stage of the cancer. The goal might be aimed for curing or palliative support only. The primary therapeutic options include:
- Surgery - if the tumor is localized, surgery is the preferred approach as the chances of cure are relatively high. If the tumor is very advanced, the surgical removal of masses is only done with the aim of relieving the symptoms, since the total cure is not possible
- Chemotherapy - usually used in conjunction with surgery and/or radiotherapy. It is particularly beneficial when the cancer has already spread to the nearby lymph nodes
- Radiation therapy - although it can be useful when combined with chemotherapy, radiation is not used very often because of the sensitivity of the bowels to high-energy radiation.
- Targeted drug therapy - typically aimed at people with advanced cancer, targeted therapies can be administered in combination with chemotherapy or as a stand-alone treatment. These drugs act on specific targets which are responsible for the overgrowth of cancerous cells. Examples of such drugs include: bevacizumab (Avastin), cetuximab (Erbitux), panitumumab (Vectibix) and regorafenib (Stivarga).











