Overview
Inflammatory Bowel Disease is a general name for medical conditions affecting part or all of your digestive tract. The digestive tract, also referred to as the gastrointestinal (GI) tract, consists of your mouth, esophagus, stomach, small intestine, large intestine, rectum, and anus.The GI tract, along with accessory organs, make up the digestive system which is simply responsible for breaking down food you consume, absorbing nutrients from the food, and eliminating unessential substances as well as toxins from the body.
Elimination by the digestive system also plays an invaluable role in immunity. However, considering the total estimated surface area of the GI tract equates to the total surface area of a football field, the digestive tract maintains an innate vulnerability to disease. As a matter of fact, counting only two of its most common forms, Inflammatory Bowel Disease currently affects close to 1% of the world's population.
Symptoms
Symptoms of IBD vary according to the location and aggressiveness of inflammation. Nonetheless, some common signs of IBD include abdominal cramping or pain, increased urgency or frequency of bowel movements, and diarrhea. Depending on your specific form of IBD, you may also experience bloody stools, unplanned weight loss, fever, and fatigue. It is very important to pay attention to these signs and quickly seek medical attention especially if you suffer from diarrhea, as more serious, life-threatening conditions like dehydration can develop.Risk Factors and Common Forms
Inflammatory Bowel Disease affects an equal number of men and women though some risk factors seem to increase your chances of developing IBD. Caucasians and Ashkenazi Jews under 30 years of age have the greatest risk, though IBD can form in individuals of any ethnicity or age. Likewise, having a parent, sibling, or child with Inflammatory Bowel Disease also increases your risk along with excessive use of isotretinoin (an acne medication), pain relievers, and cigarette smoking.Additionally, chances of getting Inflammatory Bowel Disease rise if you live in a northern, urban, or industrialized area with less than ideal environmental conditions. Scientists have excluded stress and poor diet as likely risk factors, although stress can exacerbate symptoms. Still, some insight appears to lie in studying Crohn’s disease and ulcerative colits - the two most common forms of IBD.
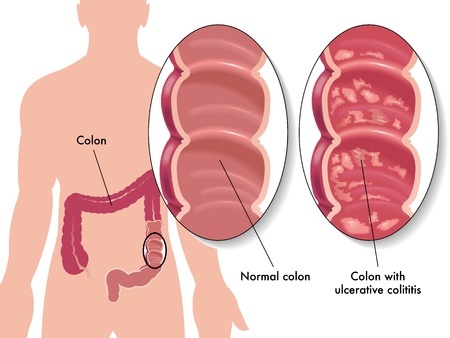
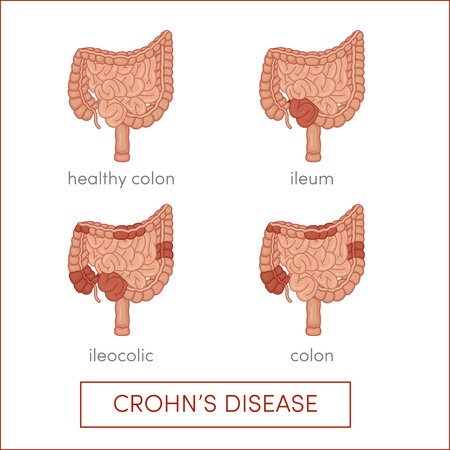
Crohn’s disease aggravates any region lining the digestive tract whereas ulcerative colitis usually affects only the lining of the large intestine and rectum. Both Crohn’s disease and ulcerative colitis are believed to be hereditary since they run in families, and research suggests these conditions could also be caused by dysfunction of the immune system.
Diagnosis
After ruling out a number of other diseases that could cause your symptoms, your doctor will conduct a series of tests to confirm diagnosis for IBD. This testing will most likely begin with taking a stool sample and blood. Respectively, these tests reveal the presence of certain white blood cells, bowel infections, bacteria, viruses, parasites, as well as anemia and antibodies. Next, your doctor may resort to his or her preferred method of imaging which may be:
- Colonoscopy
- Flexible sigmoidoscopy
- Barium enema with an x-ray
- Computerized tomography (CT) scanning
- Magnetic resonance imaging (MRI)
- Capsule endoscopy
- Double-balloon endoscopy
- Small bowel imaging
Treatment
Treating IBD effectively means attacking the disease at the source by reducing inflammation. Reducing the inflammation will in turn ease and hopefully eliminate your symptoms. This is all achieved via:- Antibiotics - these reduce drainage while healing fistulas and abscesses in Crohn’s disease patients. Antibiotics also diminish intestinal bacteria, which are capable of triggering symptoms.
- Anti-diarrheals - these fiber supplements relieve diarrhea by making your stools larger and firmer.
- Anti-inflammatory drugs - most doctors try anti-inflammatory drugs first when treating inflammatory bowel disease. These drugs work actively to eliminate inflammation, which should help relieve your other symptoms.
- Calcium and Vitamin D supplements - Crohn’s disease and medications for inflammatory bowel disease that contain steroids may cause calcium-loss from your bones and increase your risk for osteoporosis. So, your doctor may give you a calcium supplement with vitamin D to prevent this.
- Diet adjustments - again, suppressing inflammation is essential to treating inflammatory bowel disease effectively. Therefore, your doctor will provide you with a list of inflammation-inducing foods to avoid as well as a list of foods that will balance your bowels.
- Immune system suppressors - these drugs suppress the immune system in an effort to minimize inflammation. Doctors often prescribe these for patients with ulcerative colitis.
- Iron supplements - intestinal bleeding produces anemia in some patients. Thus, once your bleeding is under control, your doctor will give you an iron supplement to restore your iron levels and reverse anemia.
- Laxatives - swelling as a result of inflammatory bowel disease sometimes causes the intestines to narrow and patients to become constipated. Laxatives relieve constipation, but you should first check with your doctor to see if a certain laxative is safe for you.
- Pain relievers - for mild pain, your doctor will recommend you take acetaminophen. However, you should not take ibuprofen, naproxen, or aspirin, as they can worsen IBD symptoms.
- Surgery for ulcerative colitis - eliminates ulcerative colitis completely. It usually involves removing the entire colon and rectum. Consequently, following surgery, patients must wear a small bag over an opening in their abdomen to collect stool. But another procedure called ileoanal anastomosis allows patients not to wear an external bag. Instead, the surgeon produces a pouch from the end of the small intestine and attaches it directly to the anus allowing for more normal waste excretion.
- Surgery for Crohn’s disease - does not eliminate Crohn’s disease, but can temporarily improve symptoms. This surgery removes damaged sections of your digestive tract and connects the healthy sections. The surgeon may also use this opportunity to close fistulas, drain abscesses, and expand sections of intestine that may have narrowed.










